SDG 3 and Sustainable Recovery

Key aspects of SDG 3:
1. End epidemics and neglected diseases (target 3.3)
Ending the COVID-19 pandemic as well as preventing, treating and controlling other epidemics and diseases is essential to the enjoyment of a range of human rights.
The right to prevention, treatment and control of diseases is an integral part of the more general right to health. In this context, inequality plays a significant role in the extent to which different sectors of the population are vulnerable to, or benefit from, measures to combat and control epidemics of communicable diseases.
In terms of hospitalization, morbidity and mortality, the pandemic has disproportionately impacted racial or ethnic minorities including indigenous peoples, low-paid essential workers, migrants and refugees, older populations in care homes, incarcerated populations and homeless people.
Sustainable response and recovery actions:
All countries must take measures to contain COVID-19 while maintaining attention to other epidemics and diseases. Measures must focus on mitigating negative impacts on the human rights of all, with particular attention to the most vulnerable groups.
The crisis calls for a strategized response especially to those groups disproportionately affected.
The pandemics exposed a global health system that was inadequately prepared with insufficient resources and a lacking agility. Non-discriminatory access to testing, treatment and vaccines as well as accurate health information are essential. Furthermore, countries should apply an approach that supports all communities to have resources to promote health while minimalizing the negative impacts of social health measures.
Visit the documents and resources listed in the “Key Human Rights Guidance” below for more information.
The Universal Declaration of Human Rights (UDHR), art. 3: Everyone has the right to life, liberty and security of person.
International Covenant on Civil and Political Rights (ICCPR), art. 6.1: Every human being has the inherent right to life. This right shall be protected by law. No one shall be arbitrarily deprived of his life.
International Covenant on Economic, Social and Cultural Rights (ICESCR), art 12.1: The States Parties to the present Covenant recognize the right of everyone to the enjoyment of the highest attainable standard of physical and mental health.
International Covenant on Economic, Social and Cultural Rights (ICESCR), art 12.2: The steps to be taken by the States Parties to the present Covenant to achieve the full realization of this right shall include those necessary for: (…)
12.2.c: The prevention, treatment and control of epidemic, endemic, occupational and other diseases
2. Achieve universal health coverage and access to affordable medicines and vaccines (target 3.8, 3.b)
Inequality of access to healthcare due to prohibitive costs, location of healthcare facilities, discrimination against certain sectors of the population and other factors, has meant that vulnerable sectors of the population have been worse affected by the pandemic than others.
COVID-19 has halted around two decades of global progress towards Universal Health Coverage and significantly increased risks and vulnerabilities of those without health insurance/access to healthcare services. At least half of the world population still does not have full coverage of essential health services and about half a billion people were pushed or further pushed into extreme poverty because of health costs prior to pandemic.
Health systems are being overwhelmed by the pandemic. When health systems collapse, deaths from the outbreak itself can quickly be exceeded by deaths from preventable or treatable conditions, no longer managed by a failing health system. The pandemic has also resulted in a drop in immunization coverage (for diseases other than COVID-19) and resulted in an increase of deaths by tuberculosis and malaria.
Sustainable response and recovery actions:
It is crucial to maintain essential, lifesaving health services even while addressing the pandemic.
A full response to the COVID-19 crisis requires wide access to an extensive array of medical products and other technologies, ranging from protective equipment to contact tracing software, medicines and diagnostics, as well as vaccines and treatments.
COVID-19 vaccines must be treated as global public goods, affordable to all and accessible without discrimination. The distribution should be done through transparent protocols that respect human rights. Vaccine nationalism and hoarding must be avoided. The focus must be on ensuring equitable access to vaccines for all with attention to the most vulnerable.
Long-term recovery must aim at strengthening health systems with a focus on primary healthcare, universal health coverage and preparedness for future waves of COVID-19 and other pandemics.
Visit the documents and resources listed in the “Key Human Rights Guidance” below for more information.
The Universal Declaration of Human Rights (UDHR), art. 21.2: Everyone has the right of equal access to public service in his country
The Universal Declaration of Human Rights (UDHR), art. 25.1: Everyone has the right to a standard of living adequate for the health and well-being of himself and of his family, including food, clothing, housing and medical care and necessary social services, and the right to security in the event of unemployment, sickness, disability, widowhood, old age or other lack of livelihood in circumstances beyond his control.
International Covenant on Economic, Social and Cultural Rights (ICESCR), art. 12.1: The States Parties to the present Covenant recognize the right of everyone to the enjoyment of the highest attainable standard of physical and mental health.
International Covenant on Economic, Social and Cultural Rights (ICESCR), art.12.2: The steps to be taken by the States Parties to the present Covenant to achieve the full realization of this right shall include those necessary for:
12.2.d: The creation of conditions which would assure to all medical service and medical attention in the event of sickness.
3. Strengthen capacity for early warning, risk reduction and management, and increase health financing (targets 3.d, 3.c)
The COVID-19 pandemic has exposed gaps in early warning and preparedness systems across the world, including in high-income countries.
The vastly increased demand for healthcare has prompted an acute need for increased health financing, as well as training and protection for millions of doctors, nurses and other healthcare workers around the world. Health workers, the majority of whom are women (70%), are exposed to high risks on the frontline of dealing with the pandemic and often lack basic protection. Many countries were already far below the WHO recommended ratio of nurses and doctors per 1000 people before the surge in healthcare demand caused by the pandemic.
Sustainable response and recovery actions:
It is essential that all countries learn from the pandemic response and strengthen capacities at all levels to foresee, prevent and manage future pandemics and other global risks. Countries must use this watershed moment to invest in health emergency preparedness and critical public services including primary health care and universal health coverage. International finance institutions must provide fiscal and policy space for governments to realize the right to health, as an essential part of recovery and economic sustainability.
Visit the documents and resources listed in the “Key Human Rights Guidance” below for more information.
Universal Declaration of Human Rights (UDHR), art. 3: Everyone has the right to life, liberty and security of person.
International Covenant on Civil and Political Rights (ICCPR), art. 6.1: Every human being has the inherent right to life. This right shall be protected by law. No one shall be arbitrarily deprived of his life.
International Covenant on Economic, Social and Cultural Rights (ICESCR), art. 12.1: The States Parties to the present Covenant recognize the right of everyone to the enjoyment of the highest attainable standard of physical and mental health.
Convention on the Rights of Persons with Disabilities (CRPD), art. 11: States Parties shall take, in accordance with their obligations under international law, including international humanitarian law and international human rights law, all necessary measures to ensure the protection and safety of persons with disabilities in situations of risk, including situations of armed conflict, humanitarian emergencies and the occurrence of natural disasters.
Universal Declaration of Human Rights (UDHR), art. 27.1: Everyone has the right freely to participate in the cultural life of the community, to enjoy the arts and to share in scientific advancement and its benefits.
International Covenant on Economic, Social and Cultural Rights (ICESCR), art. 15.1.b: The States Parties to the present Covenant recognize the right of everyone: To enjoy the benefits of scientific progress and its applications;
International Covenant on Economic, Social and Cultural Rights (ICESCR), art. 2.1: Each State Party to the present Covenant undertakes to take steps, individually and through international assistance and co-operation, especially economic and technical, to the maximum of its available resources, with a view to achieving progressively the full realization of the rights recognized in the present Covenant by all appropriate means, including particularly the adoption of legislative measures.
Key Human Rights Guidance:
-
COVID-19 and Universal Health Coverage, United Nations, Policy Brief, 2020
-
Right to life-saving interventions with COVID-19, UN Special Procedures, News, 2020
-
Guidance on the Coronavirus disease (COVID-19) pandemic, World Health Organization (WHO)
-
COVID-19 Data Futures Platform, United Nations Development Programme (UNDP), website
-
COVID-19 and the Need for Action on Mental Health, United Nations, Policy Brief, 2020
-
COVID-19 Strategic Preparedness and Response, World Health Organization, Plan, 2021
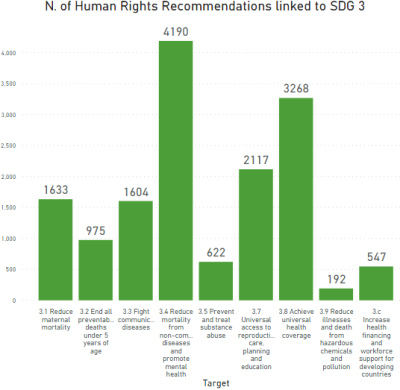
Explore all Recommendations from human rights monitoring mechanisms linked to SDG 3 by country

